Frozen shoulder, also known as adhesive capsulitis, is a condition that limits shoulder mobility due to pain and stiffness. In this post, we’ll explore what frozen shoulder is, along with its symptoms, causes, and treatments.
Key Takeaways
- Frozen shoulder, or adhesive capsulitis, is characterized by pain and stiffness that severely restricts shoulder movement.
- The condition progresses through three stages: freezing, frozen, and thawing, each with distinct symptoms and durations that can span months to years.
- Non-surgical treatments like physical therapy and corticosteroid injections are often effective for managing symptoms. Surgery is an option for severe cases that do not respond to conservative methods.
Understanding Frozen Shoulder (Adhesive Capsulitis)
Frozen shoulder, or adhesive capsulitis, is a shoulder condition that causes pain and stiffness in the shoulder joint. It can severely restrict movement, making everyday tasks like reaching for a high shelf or getting dressed in the morning difficult.
The condition results from the thickening and tightening of the strong connective tissue surrounding the shoulder joint, known as the shoulder joint capsule. This process leads to the formation of scar tissue, which limits the joint’s range of motion.
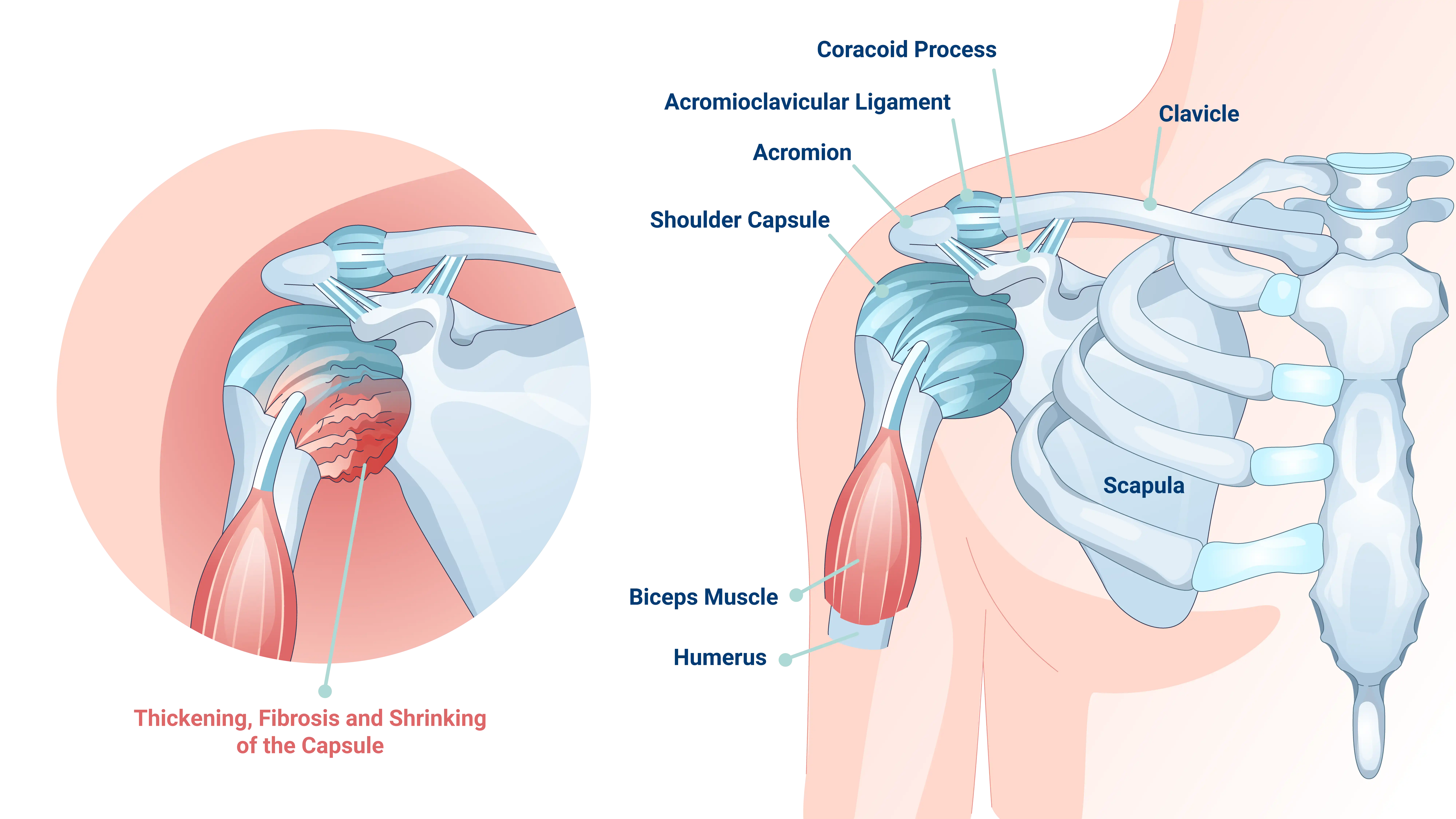
Frozen shoulder can develop gradually, sometimes without a clear cause, but it is frequently seen following an injury or surgery. Understanding the underlying mechanisms helps inform both management and treatment strategies.
Stages of Frozen Shoulder
Frozen shoulder typically progresses through three distinct stages: freezing, frozen, and thawing. Each stage has its own set of symptoms and duration.
The freezing stage can last anywhere from 2 to 9 months and is characterized by increasing shoulder pain and a gradual loss of shoulder movement. During this stage, the pain worsens at night and may disrupt sleep.
Following the freezing stage is the frozen stage, which may last from 4 to 12 months. In this period, shoulder pain might decrease, but the stiffness remains and continues to restrict mobility.
Finally, the thawing stage marks the gradual recovery of shoulder movement, which can take anywhere from 5 to 24 months.
Knowing this progression helps set realistic expectations for recovery and guides appropriate treatment planning.
Common Symptoms of Frozen Shoulder
The symptoms of frozen shoulder may vary depending on the stage of the condition. Recognizing the initial set of symptoms can lead to prompt diagnosis and treatment. Early symptoms include:
- Persistent pain in the shoulder
- Stiffness that makes it challenging to move the shoulder joint, leading to a limited range of motion
- Worsening pain at night, which can interfere with sleep and overall quality of life
These symptoms can interfere with everyday activities such as dressing, reaching, or lifting. Early recognition of these symptoms is key to seeking timely medical intervention and preventing further deterioration.
Causes and Risk Factors
Several factors can increase the risk of developing frozen shoulder. One of the most significant risk factors is age, with individuals over 40 years old being more susceptible. Women are also at higher risk of developing this condition.
In addition to age and gender, certain medical conditions can elevate the likelihood of developing frozen shoulder. These include diabetes, thyroid disorders, cardiovascular disease, and Parkinson’s disease.
Prolonged shoulder immobility, often due to injuries or surgery, can also contribute to frozen shoulder. When the shoulder is kept still for extended periods of time, the capsule surrounding the joint may thicken and tighten, leading to the development of this condition.
Recognizing these risk factors allows for early intervention and preventive strategies, particularly in high-risk individuals.
Diagnosing Frozen Shoulder
Diagnosing frozen shoulder typically involves a combination of clinical evaluation and, when necessary, imaging studies to rule out other conditions.
The clinical evaluation includes a thorough medical history and a physical examination. You will discuss any symptoms that you’ve noticed, as well as any past injuries or medical conditions. During the physical exam, your doctor will check for signs of pain, stiffness, and limited range of motion in the shoulder joint.
Imaging tests like X-rays and magnetic resonance imaging (MRI) can help exclude other potential conditions such as arthritis or bone abnormalities.
This comprehensive approach ensures an accurate diagnosis, essential for developing an effective treatment plan.
Non-Surgical Treatments for Frozen Shoulder
Non-surgical treatments are often the first line of treatment for frozen shoulder, focusing on easing pain and improving shoulder motion.
Physical therapy is the cornerstone of non-surgical treatment. Patients are guided through specific exercises aimed at improving the range of motion and reducing stiffness. For best results, it is important to stay consistent and closely adhere to the physical therapy program.
Corticosteroid injections may be used to reduce inflammation and relieve pain, particularly in the early stages. These can improve shoulder function and allow better participation in physical therapy. Another treatment option is hydrodilatation, which involves injecting sterile water into the shoulder joint to help stretch the tissue and improve movement.
Pain management is essential for treating frozen shoulder. Nonsteroidal anti-inflammatory drugs (NSAIDs) may be recommended for short-term use. Heat or cold compresses can ease pain and stiffness, making it easier to perform therapeutic exercises.
These non-surgical treatments can be highly effective in managing frozen shoulder. In some cases where these treatments do not relieve symptoms, surgery may be recommended.
Surgical Options for Severe Cases
Surgery is rarely required for frozen shoulder, but may be necessary in cases. It may be considered for individuals with persistent symptoms and significant loss of shoulder mobility. Surgery should be performed by an experienced shoulder specialist.
Common surgical options include manipulation under anesthesia and shoulder arthroscopy. Shoulder manipulation is performed under general anesthesia to free up restricted movement by breaking up the scar tissue within the shoulder joint. Arthroscopic surgery is a minimally invasive technique used to remove scar tissue and release the tight joint capsule.
The goal of surgery is to alleviate tightness in the joint capsule and restore shoulder movement. Recovery following frozen shoulder surgery can vary, generally taking anywhere from six weeks to three months. Post-surgery physical therapy is necessary for proper healing and regaining strength and flexibility. Continued commitment to rehabilitation is essential for regaining maximal function.
Preventing Frozen Shoulder
Taking preventive measures can reduce the risk of developing frozen shoulder. These include maintaining regular shoulder movement and avoiding prolonged immobilization.
Incorporating gentle stretching exercises into your regular routine helps keep the shoulder joint flexible. Patients recovering from injury or surgery are encouraged to begin their physical therapy programs and move the shoulder as soon as it’s safe to do so.
These preventive steps can lower the likelihood of developing frozen shoulder and reduce the severity of symptoms if it does occur.
Summary
Frozen shoulder, or adhesive capsulitis, is a condition that causes significant pain and stiffness in the shoulder joint, affecting daily activities and overall quality of life. Understanding the stages of frozen shoulder and recognizing the common symptoms can help in seeking timely medical intervention.
Non-surgical treatments, such as physical therapy, corticosteroid injections, and hydrodilatation, play a key role in managing the condition and improving shoulder movement. In severe cases, surgical options like shoulder manipulation and arthroscopy may be necessary to alleviate symptoms and restore function.
Preventing frozen shoulder involves maintaining regular shoulder movement and avoiding prolonged immobilization. With early intervention and appropriate treatment, individuals can expect a gradual recovery and return to normal activities. Remember, patience and commitment to therapy are key to overcoming frozen shoulder.
Frequently Asked Questions
What is frozen shoulder?
Frozen shoulder, or adhesive capsulitis, is a painful condition that results in stiffness and restricted range of motion in the shoulder joint. This limitation can severely affect daily activities and overall quality of life.
What are the stages of frozen shoulder?
Frozen shoulder progresses through three stages: the freezing stage, where pain increases and mobility decreases; the frozen stage, characterized by stiffness; and the thawing stage, during which range of motion gradually improves. Understanding these stages can help in managing the condition effectively.
How is frozen shoulder diagnosed?
Frozen shoulder is diagnosed through a comprehensive patient history, physical examination, and possibly imaging tests to exclude other conditions.
What are the non-surgical treatment options for frozen shoulder?
Non-surgical treatment options for frozen shoulder include physical therapy, corticosteroid injections, hydrodilatation, and pain management techniques. These methods can effectively alleviate symptoms and improve mobility.
How can I prevent frozen shoulder?
To prevent frozen shoulder, it’s essential to maintain regular shoulder movement, avoid prolonged immobilization, and incorporate gentle stretching into your routine. This proactive approach will help keep your shoulder muscles and joints flexible.

